Most health service organisations will find themselves in need of a temporary infrastructure solution at some point, either because of a planned event, such as refurbishment of the existing facility; or an unexpected event, the Covid-19 outbreak being a recent example. But while modular facilities often provide the answer to a temporary issue that requires a quick resolution, that doesn’t mean the solution has to be short-term. Why use a modular facility? A common reason for commissioning a temporary solution is insufficient capacity or a spike in demand, due to seasonal pressures or another temporary reason, which can present a risk of compromised care standards and patient dissatisfaction.
The need to maintain high standards of patient care, compliance and safety throughout a refurbishment or service reconfiguration project, or during an unforeseen event such as Covid-19, is another reason additional healthcare infrastructure may be required.
However, it’s not all about being able to respond to an urgent need or crisis; temporary healthcare facilities are also an essential component of strategic plans. Although the very nature of emergencies means that they are unpredictable, planning for different scenarios using flexible and adaptable solutions is essential.
A modular building can also be used to pilot new surgical delivery methods, new models of care delivery or new technology and equipment without risk to existing routines, and can also enable health service organisations to deliver community-based diagnostics and care outside of the acute hospital setting. This makes them a potentially core element of planned Community Diagnostic Hubs. Adding capacity Whenever waiting times increase due to a temporary fall in activity for any reason - such as the recent suspension of all non-urgent surgery in many countries following the Covid-19 outbreak - a modular facility can add much needed extra capacity.
Even once the service resumes to normal levels, it can become difficult to get on top of waiting lists. To use an example from the current pandemic; the need to retain significant capacity in Australian hospitals for a potential influx of Covid-19 patients meant providers in some states were ordered to limit elective surgery at 50% or 75% of previous room capacity. A temporary modular healthcare facility could add sufficient capacity to bring this back up to 100%, or even above this level.
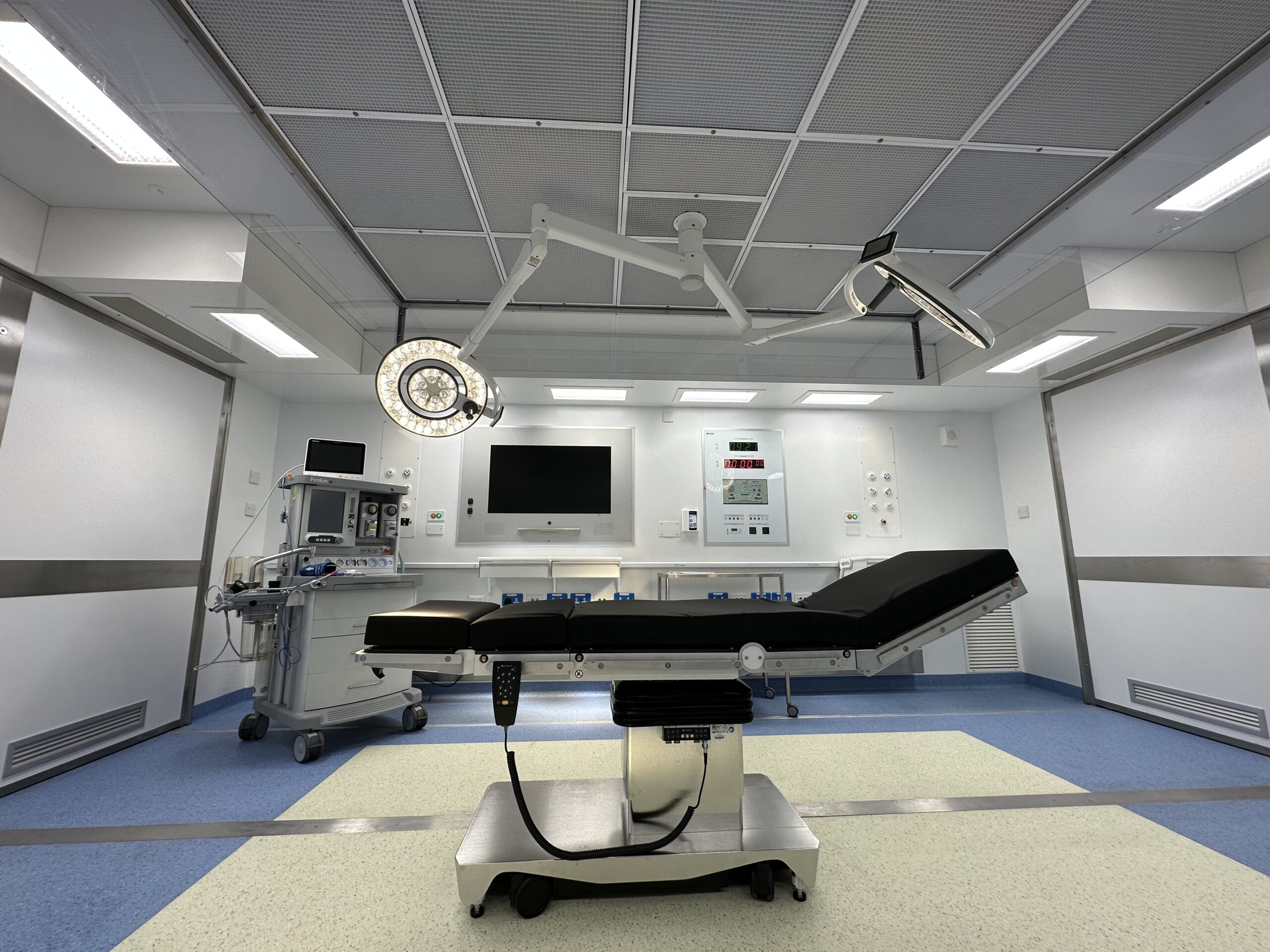
Temporary and semi-permanent stand-alone operating rooms can be set up and connected to the main hospital very quickly. Equipped with air conditioning systems that allow variable humidification, modular rooms also incorporate IPS, UPS, integrated water system and medical gas bank, vacuum and scavenging systems, and an environmental control system ensuring temperature, humidity and sanitation are always optimal.
Completely stand-alone, so called ‘cold’ sites for surgery, are also being set up using modular infrastructure during the pandemic. A combination of an operating room and a hospital ward can create a visiting hospital, which provides a complete clinical environment including an anaesthetic room, scrub and recovery areas, clean and dirty utility areas, a reception/nurse station, waiting room, ward and WC.
 Reassuring patients
Modular wards are being used during the pandemic not only to supply additional hospital bed spaces, but also to provide additional reassurance for patients. This was the case at Kettering General Hospital in the UK, which commissioned a modular ward at the start of the pandemic to provide a Covid-free zone.
Reassuring patients
Modular wards are being used during the pandemic not only to supply additional hospital bed spaces, but also to provide additional reassurance for patients. This was the case at Kettering General Hospital in the UK, which commissioned a modular ward at the start of the pandemic to provide a Covid-free zone.
As well as providing the hospital with temporary additional bed capacity for non-Covid patients, the 18-bed modular ward offers reassurance for at-risk patients who may have been worried about attending hospital during the pandemic. The facility will remain on site for an initial period of 6 months, meaning Covid-19 capacity can be retained within the hospital in case of a second wave.
The modules were built off-site by Young Medical , Q-bital’s specialist modular subsidiary, and the stand-alone ward facility was completed within a period of just five weeks, despite the restrictions imposed by the lockdown protocol that was in place at the time. Delivering new models of care To deliver fully integrated community-based healthcare, flexibility is required. A modular outpatient clinic can offer the opportunity to care for and process outpatients in the heart of their own communities, either on an ongoing basis or as part of a specific programme.
In terms of healthcare service delivery, one concept that is being implemented widely in areas where accident & emergency departments are under particular pressure, is the separation of urgent cases from patients with less serious injuries or ailments, either on a temporary or a more permanent basis, to improve patient flow.
To effectively reconfigure a service, buildings and facilities often need to be adapted. Setting up a temporary modular facility can allow hospitals to test out scenarios before investing significant amounts of money in a new or remodelled permanent building. Enabling rapid response Temporary healthcare facilities can also enable hospitals to respond quicker to a crisis or emergency. One of the most recent examples is the priority assessment spaces or isolation pods, created with the intention of preventing patients with suspected Covid-19 who arrive at the hospital from mixing with vulnerable patients. In many cases, hospitals also had an urgent need for extra space to house staff and changing areas.
Modular units like these can remain on for an indefinite period, and can be moved, repurposed or handed back when they are no longer needed. But modular facilities are often designed to be in place for much longer than that.
 Ensuring uninterrupted care
A less dramatic but more common reason for using modular is the need to minimise disruption to healthcare services during a reconfiguration of departments or a refurbishment programme. Where a major project is taking place, there may even be a need for a bespoke semi-permanent building.
Ensuring uninterrupted care
A less dramatic but more common reason for using modular is the need to minimise disruption to healthcare services during a reconfiguration of departments or a refurbishment programme. Where a major project is taking place, there may even be a need for a bespoke semi-permanent building.
This was the case for Skåne University Hospital (SUS) in Malmö, which is currently undergoing a major construction programme that is estimated to take seven to ten years to complete. The hospital is Sweden’s third largest and it represents one of two national centres for cardio-thoracic surgery.
During the build, an urgent need arose for increased capacity for performing high-risk orthopaedic procedures, and the hospital’s management wanted an interim solution that would be quick to implement, while being robust enough to fill the gap until the new building was complete.
Young Medical provided the hospital with a 324 m2 operating room complex to strict requirements, including an ultra-clean air system, the latest surgical lights and a bespoke building management system. The interim facility was to be integrated with the existing operating room department on the third floor of the hospital to ensure a seamless extension, something that involved a precision engineered steel construction that was fixed at the exact same height as the existing facility.
The entire project was completed within just 10 months from start to finish, and while commissioned as an interim facility, the complex is designed to serve the hospital for a period of up to ten years. More than just a temporary building The use of modular construction techniques and volumetric buildings in the healthcare sector is not new; offsite manufacturers have supplied healthcare buildings for many years. However, modular is often seen as just a ‘box’ or ‘shell’; a short-term solution that is necessary but basic, and that may look unsightly.
Over the past decade, the modular concept has moved on and a range of different solutions can be achieved; from a basic container concept to bespoke, sophisticated facilities housing fully equipped operating rooms that can be integrated with the existing hospital’s own infrastructure if required.
Modular solutions don’t have to be temporary; it is possible to have a permanent extension to an existing hospital built entirely using a modular concept, and designed to fit seamlessly with the rest of the building.
Mobilising flexible infrastructure can support hospitals in; maintaining control of the patient pathway, preventing operational downtime, reducing build and refurbishment project time scales and facilitating uninterrupted patient care. A modular solution is also usually much quicker to implement, can deliver cost savings, and provides a more sustainable option compared with a traditionally built healthcare building.
For further detail on modular healthcare buildings, please visit www.q-bital.com or contact [email protected]


Q-bital Healthcare Solutions
Unit 1144 Regent Court, The Square, Gloucester Business Park, Gloucester, GL3 4AD
