Innovative solutions that help to create capacity and allow more efficient working are key to facilitating the Covid-19 recovery process.
An article published towards the end of 2021 in the British Journal of Healthcare Management suggests mobile or modular healthcare facilities, which provide flexible and cost-effective spaces to expand services without sacrificing care quality, may be the solution to both the patient care and building maintenance backlogs within the NHS. But the issue is not specific to the UK; other countries are facing similar challenges and are dealing with inflated waiting lists and healthcare inequalities. A need for capacity Capacity is becoming an increasingly pressing problem for healthcare services at a time when demand is increasing. Although the situation differs between countries, many countries across the globe are seeing their population both ageing and increasing in numbers. The Nuffield Trust has estimated that in the UK alone, the equivalent of 22 new hospitals with 800 beds each will be needed by 2027 to accommodate population growth and a rising proportion of older people.
This has a number of implications; not only are older people more likely to live with multiple long-term conditions, hospital bed occupancy levels also increase towards the end of life, putting additional pressure on hospital beds.
Right now, the most urgent issue is that healthcare systems continue to be disrupted by the Covid-19 pandemic, having a knock-on effect on elective surgery waiting lists and other non-urgent treatments. It is not unusual to see waiting times being more than two years for hip and knee replacement surgery, for example. As well as being distressing for the individual, this delay in surgery can lead to an increased risks of falls, fractures and other adverse events, which can result in increased pressure on healthcare services.
Even more worrying, articles have suggested that urgent category-one elective surgeries have also been postponed because of the increasing shortage of beds in hospitals and the need to make room for Covid-19 patients. Diagnostic services have also been impacted negatively; for example, estimates from the Victorian Cancer Registry in Australia reportedly show almost 3500 cancers were missed between April last year and mid-August this year, half of which were for prostate cancer.
There is an urgent need for innovative solutions to increase capacity in hospitals. With patient backlogs mounting, ‘future proof’ health infrastructure plans taking a more flexible approach to creating and configuring space in the healthcare sector are needed.
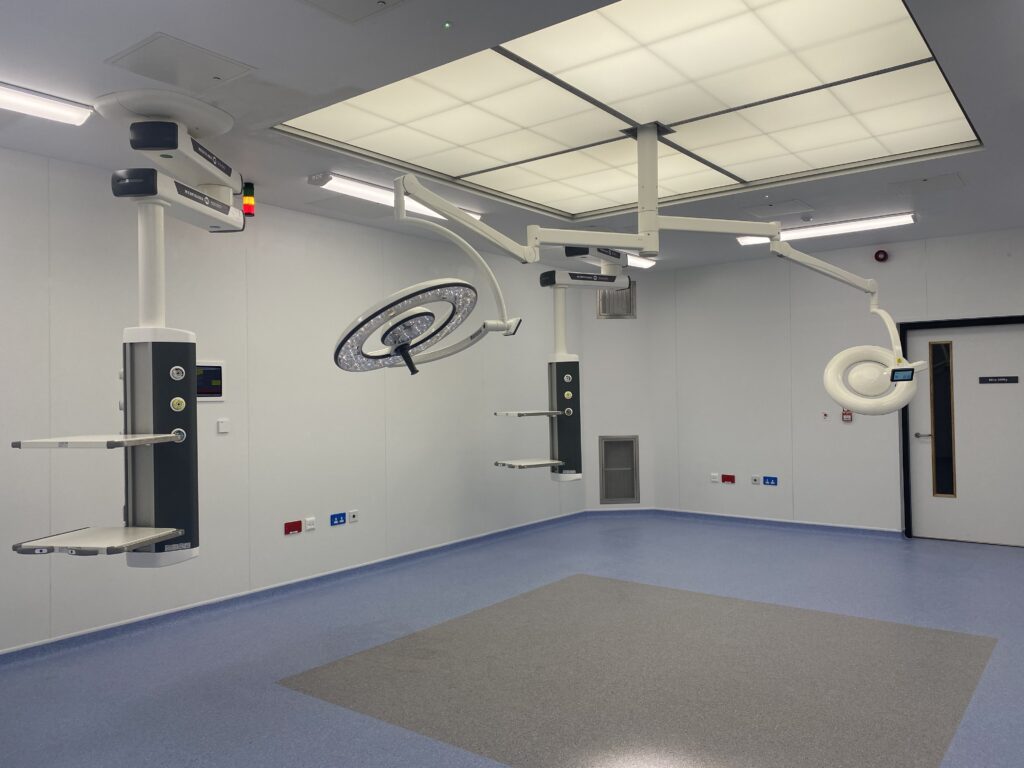
What are flexible healthcare facilities?
Modular health facilities are constructed from individual, largely prefabricated modules that are then installed on to a site to create a single structure, or series of structures. They can be used as stand-alone facilities on a particular hospital site, attached to an existing hospital building or used in conjunction with a mobile facility.
While modular facilities can be designed specifically for the particular healthcare function they are required for, mobile facilities can be moved between different locations in line with variations in demand. With appropriate maintenance, both modular and mobile facilities can last up to 60 years.
Modular building methods have been used in social housing and education for several decades as a faster and more cost-effective way of creating space. In a healthcare context, they have typically been used to increase capacity in times of high demand or to provide space to continue services while an existing building is being renovated or refurbished.
The healthcare field is well-suited to modular design, as facilities usually include functional elements that have clear pre-existing procedures and standards, and the Covid-19 pandemic has highlighted the role that modular facilities can play in healthcare. As stand-alone buildings, modular facilities can allow patients who test positive for the virus to be kept entirely separate from the main hospital building.
Using this approach, a cataract surgical unit at Stoke Mandeville in the UK installed a modular unit to act as a COVID-free zone, allowing the surgical team to become one of the first services to re-start elective procedures after the initial pause during lockdown. Since then, many other hospitals have followed suit. In Brisbane, Australia, the installation of a mixed-modality colonoscopy unit is allowing 6,600 extra screening procedures to be performed per year, facilitating faster detection of one of the country's most common cancers.

Healthcare technology, clinical practice and policy can develop very quickly, so building projects that take many years are at risk of being out of date before they are even finished. The rapid adoption of healthcare technology during the Covid-19 pandemic further highlighted the need for greater flexibility.
Both governments and healthcare providers are increasingly looking to create more flexible facilities to meet fluctuating capacity demands and deliver integrated care. Modular facilities are a good solution for this, as they can be developed far more quickly than traditional, bricks and mortar buildings, while mobile operating rooms can be moved between locations according to demand.
For example, the construction of four modular operating rooms, a ward and support hub recently built at Queen Mary's Hospital in South-West London, UK, took only 12–14 weeks from commission to completion and receiving first patients. This was possible, in part, because modular facilities need less in terms of groundworks and other enabling works, and those works that are needed can be undertaken at the same time as the off-site construction of the modules.
Flexible, mobile or modular facilities can also be removed or repurposed when demand shifts. This provides more flexibility when making planning decisions as it is possible to measure the value for money over a shorter period of time. Furthermore, fast project delivery is crucial to success in infrastructure construction and expansion, both in terms of cost saving and risk reduction.
A key element of a modular facility is that the majority of construction takes place off site. Once ready, the facility will be delivered to the site, installed and tested for quality so that the health service is left with a completed building that is ready to use immediately. Building infrastructure in a factory environment typically allows for better quality control and more efficient use of labour and resources than would be the case with on-site building.
Some modular suppliers offer leasing contracts that include regular quality standard testing, maintenance and full facilities management packages. This means there are set costs to budget for, without needing to factor in extra, unknown maintenance costs. The designs are also compliant with technical requirements meaning that hospital staff can trust the facilities’ appropriateness and safety.
In terms of the construction process, modular builds can also improve efficiency. A US study found that a modular, pre-fabricated construction approach resulted in time savings of 45%, cost savings of 16% and an increase in productivity of 30%. Further cost savings can be achieved once construction is complete, as temporary modular facilities can reduce the need to outsource to the private sector.
A common misconception about modular facilities is that they are less comfortable or customisable than a traditional hospital building. In fact, given the limitations often placed on older hospital buildings, the opposite is often true. Although the earlier models of modular building used in the 20th century were often relatively basic, more recent models are made to be bright, airy and spacious, with many options for customisation or even bespoke design.
The ability to standardise modular facilities can be a significant benefit, as it means that the layout and storage of equipment in each room can be the same, making it easier for staff to work in different rooms. These studies, alongside anecdotal evidence from healthcare staff, suggest that modular facilities are just as, if not more, comfortable and easy to use as traditional healthcare buildings. Reduced environmental impact Healthcare services contribute a significant amount of global carbon emissions; if the healthcare sector were a country, it would have the fifth highest carbon emissions in the world, along with a large amount of waste material. Because of their flexible nature, modular healthcare facilities can help to facilitate a more circular economy—a regenerative closed loop that prevents waste and promotes optimisation of physical, financial and human resources.
Off-site prefabrication is also believed to reduce construction waste and facilitate better building insulation, improving energy efficiency. This is in addition to the reduction in emissions from transporting building materials to the hospital site, as well as the noise pollution and disruption to local communities that often occurs during long on-site building projects.

Conclusion
Many of the issues that were already affecting the healthcare system - such as patient backlogs - have been exacerbated to unprecedented levels as a result of the Covid-19 pandemic. However, innovative solutions that can help to create capacity and allow more efficient working are key to facilitating the recovery process, as well as improves and prepares it for future challenges.
There is also substantial potential to address healthcare inequalities, by facilitating greater cohesion between services and local provision of both diagnostics and treatment, allowing patients to access care closer to home. Achieving this requires better integration between primary, secondary, tertiary and social care services, and it can also have major implications on existing physical infrastructure. A flexible modular or mobile facility could solve the immediate challenges.
In summary, there are a number of benefits to modular and mobile healthcare facilities, including greater flexibility, faster delivery, enhanced patient and staff experience, cost-effectiveness and a reduced environmental impact. Healthcare services experiencing capacity issues should seriously consider modular or mixed-modality facilities as an effective means of increasing capacity and/or continuing services during periods of change. A version of this article was first published in the British Journal of Healthcare Management, Vol 27, No 9 in September 2021.



Q-bital Healthcare Solutions
Unit 1144 Regent Court, The Square, Gloucester Business Park, Gloucester, GL3 4AD
